Equine Veterinarian Injury Risk: Why Dangerous Work Has Become “Normal” in Equine Practice
Every equine veterinarian knows their job can be dangerous – and the equine veterinarian injury risk is far higher than most people realise. Handling a half-ton animal that may panic or kick is “just part of the job” for many large animal veterinarians.
Over time, a culture develops where frequent injuries are accepted as routine – even inevitable – in equine practice.
Recent research and sobering statistics, however, have begun to shine a spotlight on just how common and severe these injuries are, and why the profession is starting to push back against the status quo of risk normalization.
This is a conversation I didn’t originally plan to write, but a recent accident made it impossible to ignore. I was lucky. I walked away with two black eyes and a sore head, nothing more. Many of our colleagues haven’t been so fortunate.
That experience prior to Christmas 2025 forced me to pause and reflect on how easily risk becomes routine in equine work, and how rarely we stop to question it.
So before diving into the data and the wider discussion, it’s worth asking: why have we come to accept this level of risk as normal – and what can we do differently?

Alarming Injury Rates Among Equine Vets
Multiple studies confirm that equine veterinary medicine is one of the most injury-prone occupations. In fact, being an equine vet has been deemed “the most dangerous civilian profession” in the United Kingdom (and I’m sure none of the equine veterinarians reading would disagree.)
Consider these eye-opening statistics:
- Nearly all large-animal veterinarians suffer injuries: Surveys show over 90% of equine and farm animal veterinarians have been injured at work during their careers. One United States survey in 2025 similarly found 96% of equine vets had sustained a work-related injury. By comparison, veterinary jobs overall have about five times the national average rate of workplace injuries.
- Frequent injuries over a career: A British Equine Vet Association report estimated equine vets will sustain 7- 8 significant injuries over a 30-year career – roughly one serious incident every 4 years. (I’m currently at 6 incidents in 23 years of practicing (car crash, kicked in the knee, kicked in the face, torn rotator cuff, head trauma with black eyes and getting my hand stuck in a slam gate). I consider myself very careful, yet the numbers don’t lie.
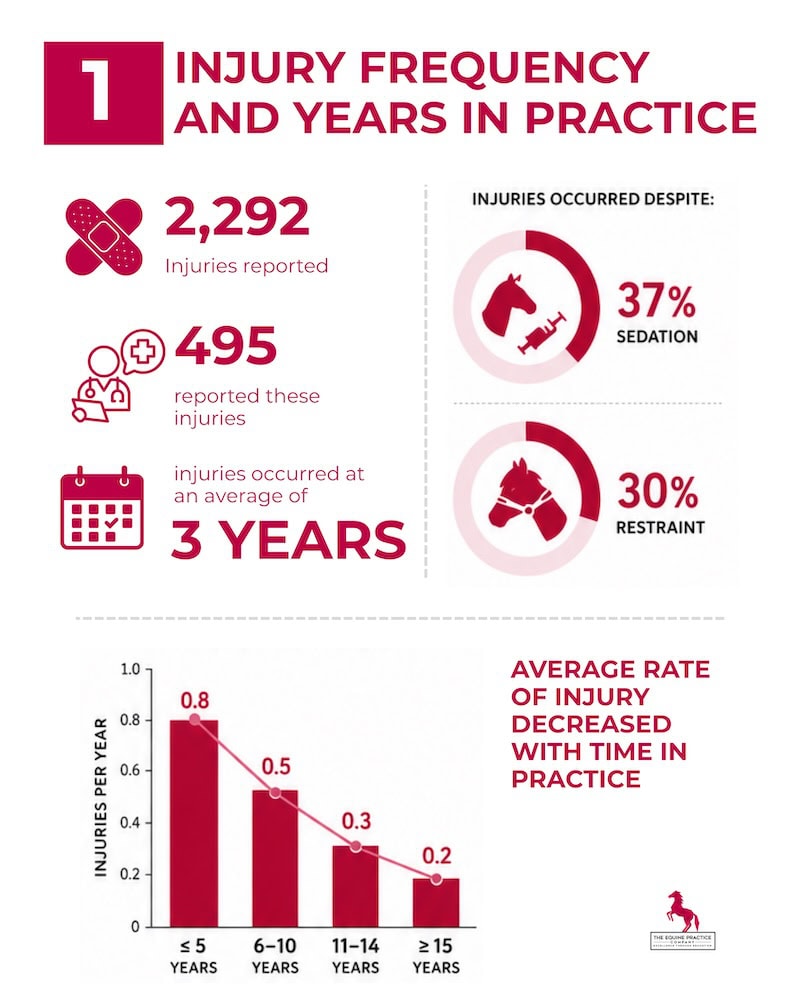
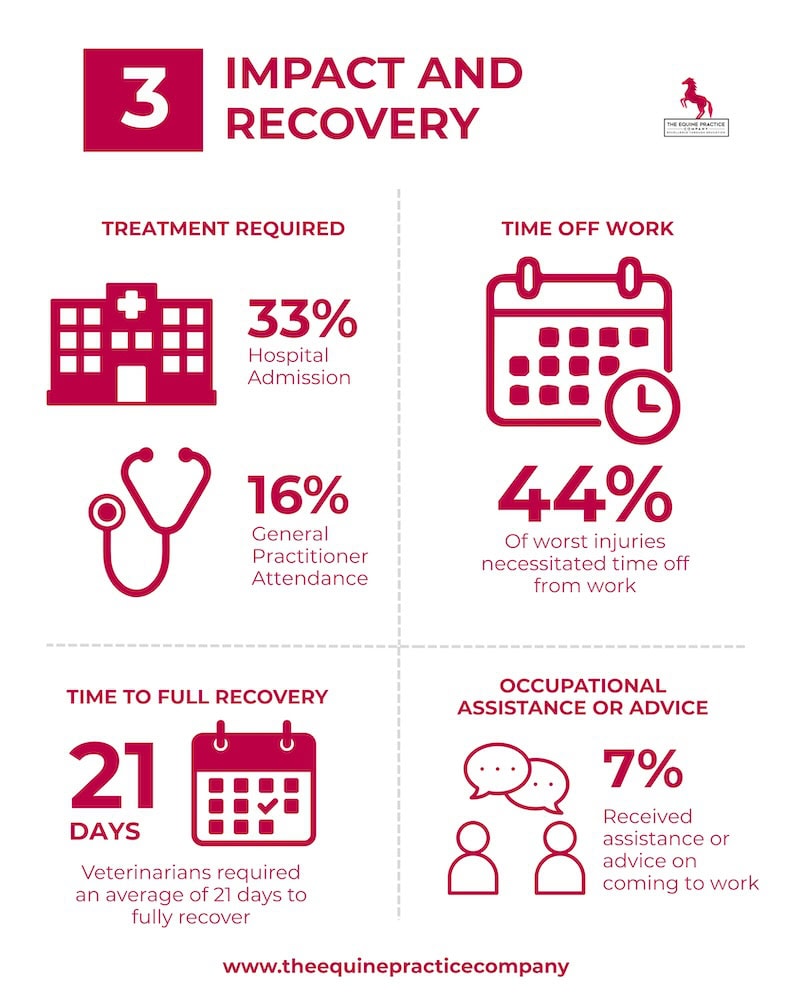
A 2018 UK survey of 620 equine veterinarians tallied 2,292 total injuries, averaging to one injury per vet every 3.7 years. In the United States, it’s reported that equine practitioners average about eight major injuries in a career, making it the second-highest profession for non-fatal injuries in the country. - High risk of hospital visits: Roughly 1 in 4 equine vet injuries is serious enough to require hospital treatment. British veterinary research found 25–33% of reported equine vet injuries led to hospital admission.
In another recent North America survey, 48% of equine vets said they had visited an ER due to a work injury, and about 12–18% had been hospitalized for their injuries. Broken bones are not uncommon – about one-third of vets had sustained a fracture on the job. - Frequent head trauma: Because so many injuries involve horses’ legs or hooves, head injuries are a major concern. An estimated 52% of equine vets have suffered some form of head or face injury in their work – from cuts and black eyes to concussions.
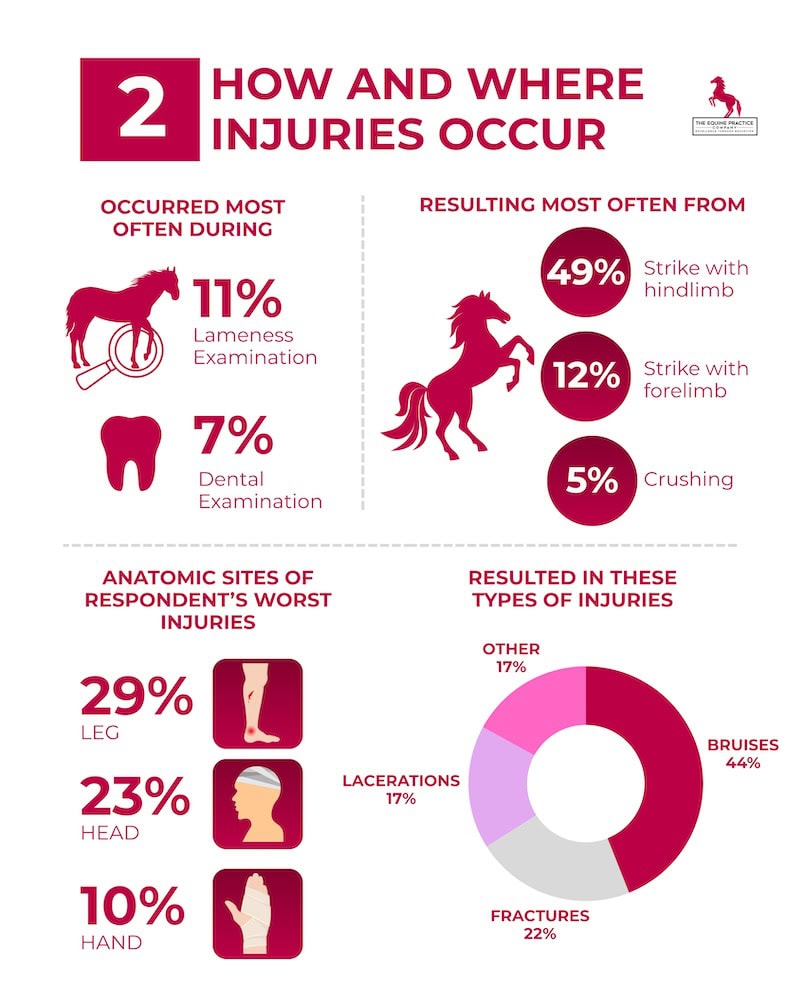
One U.K. study noted head trauma (often from being kicked while examining a horse’s legs) is among the most common injuries leading to hospital visits. Indeed, 7% of equine vet injury reports involved loss of consciousness (e.g. being knocked out by a kick). - Multiple injury mechanisms: In surveys, 89% of equine vets reported being kicked by a horse’s hind limb at some point, and about 75% had been stuck by a forelimb strike. Over 70% had been bitten by a horse, and a similar percentage had been crushed or struck against a wall by a patient.
The typical serious injuries include being kicked, stepped on, head-butted, or crushed, resulting in anything from bruises and lacerations to torn ligaments, fractures, and concussions.
These numbers make it clear that injuries are not freak occurrences – they are a near certainty in equine practice.
For context, the U.S. Bureau of Labor Statistics finds the veterinary services industry has one of the very highest nonfatal injury rates of any job (10–14 injuries per 100 workers annually, versus ~2.5 per 100 for all industries).
In the British Isles, veterinarians have a higher annual injury rate than even construction workers or prison officers. Equine vets, who handle large unpredictable animals daily, bear the brunt of that risk.
Why Risk Feels “Normal” in Equine Practice
Despite the alarming prevalence of injuries, many incidents go unreported and unaddressed due to cultural norms in the profession. This same culture of minimising harm doesn’t just affect physical safety – it also has serious consequences for veterinarian mental health, which we explore in depth in a separate article.
A recent study on safety culture titled “It’s only a flesh wound” found a widespread attitude among large-animal vets of minimizing injuries and accepting risk as part of the job. Key findings illustrate this mentality:
- Underreporting injuries: Most veterinarians in the study admitted they did not officially report injuries (even serious ones) to their employer or authorities. Injuries were often seen as “everyday” occurrences not worth the paperwork.
Many veterinarians felt that unless an incident was truly catastrophic, reporting it would have no meaningful outcome and might even be viewed as complaining. As a result, official injury statistics likely undercount the true injury rate in vet practice. - High pain tolerance and guilt: Veterinarians frequently continue working through injuries. Over 90% of injured large-animal vets in one survey took little to no time off after a significant injury. Why? Many felt guilty about burdening colleagues or letting clients down, and they downplayed the severity of their injuries.
One veterinarian quipped that as long as an injury wasn’t “gushing blood,” they’d just patch themselves up and finish the day’s calls. This tough-it-out mindset means even hospital-worthy injuries are often brushed off. - “Acceptable” hazards: Equine and farm veterinarians tend to have a higher threshold for defining an incident as an injury. One study noted that companion-animal vets might consider a dog bite that breaks skin to be an injury, whereas an equine vet might view a bruising horse kick as “part of the day” unless it truly incapacitates them.
In other words, hazards like horse kicks are seen as everyday risks, not incidents to fuss over. This normalisation leads to less reporting and less discussion about prevention. - Impact on young professionals: Newer graduates often enter a workplace culture where everyone has a story of being hurt and keeps working anyway. This can pressure young vets to think they too should “grin and bear it” after an injury.
In one survey, more than a quarter of vets said they now suffer chronic pain or physical limitations from past work injuries, yet only 2% left equine practice entirely as a result.
The vast majority stay in the field and simply live with the repercussions, reinforcing the notion that enduring injury is just part of being an equine vet.
All of this fosters a dangerous cycle: vets expect to get hurt, don’t report or rest after getting hurt, and thus take fewer steps to prevent getting hurt. When injuries are an assumed reality, the urgency of safety measures can get lost.
As Dr. John Tulloch, who led a large UK study on vet injuries, put it: “This study exposes a culture in large animal veterinary workplaces that normalises injuries and undervalues safety”. Breaking out of that culture is a major challenge now facing the profession.
When Routine Work Turns Tragic
It’s important to note that while most veterinary injuries are non-fatal, the worst-case scenarios can be truly tragic. Serious incidents – though relatively rare, serve as stark reminders of what’s at stake when handling powerful animals:
- Fatal accidents: Workplace fatalities do occur in animal care fields, and horses are a leading cause. U.S. labor data from the 1990s showed an average of 63 fatal animal-related injuries to workers per year (across all animal-related jobs), with horses being the #2 cause of these deaths (second only to cattle).
Within the racing industry, for example, 14 of 17 on-site fatalities over a period were due to horse kicks. Veterinarians themselves are not immune. About a decade ago, a U.S. equine vet died from severe head trauma while working with a stallion (the horse struck his head).
And in 2014, Irish veterinarian Dr. Gerry Long was tragically killed by a kick to the head from a client’s horse. His death helped spur the “Think Ahead” safety campaign in the United Kingdom to promote helmet use for vets.
These heartbreaking cases underscore that a split-second accident with a horse can be literally life or death. - Life-altering injuries: Even non-fatal incidents can end careers or cause lasting disability. Equine veterinarians have reported injuries resulting in lost eyes, shattered limbs, or permanent spinal damage. One survey found that over 2% of equine vets had been permanently disabled (unable to continue equine practice) by a work injury.
In other cases, veterinarians needed surgeries and months of rehab – for instance, repairing a traumatic shoulder dislocation that put a vet out of work for half a year.
It is sobering that 1 in 4–5 equine veterinarians will suffer some chronic physical problem from an on-the-job injury. The toll extends beyond the physical; such incidents can cause psychological trauma, anxiety, or loss of confidence when working around horses afterward. - Close calls are common: Talk to any equine veterinarian at a conference and you’ll hear about all the recent near-misses – the charging mare that just missed the vet, the stallion that reared and came down inches away.
Many equine practitioners have had a moment where “I realized I could have been killed just then.” These stories circulate as cautionary tales, yet they’re also passed around with a nervous laugh, reinforcing that every veterinarians has war stories.
Opening a discussion about these near-misses (and not just the worst injuries) could help others learn and adopt safer practices before another close call becomes a catastrophe. (especially the new graduates who are starting their in our occupation.
Hearing about fatalities or severe injuries in our field is always jolting – it cuts through the normalization. It reminds us that no matter how experienced or careful you are, unpredictable animal behavior can change everything in an instant. That reality is driving new conversations about improving safety.
Helmets and Safety Initiatives: Changing the Culture
The good news is that the profession is starting to respond. Protective equipment and new safety policies are slowly making their way into equine veterinary culture, challenging the old “tough it out” mindset.
The most high-profile change has been the push for wearing helmets during equine exams and procedures:
- UK leads with mandatory helmets: In 2025, one of the United Kingdom’s largest veterinary groups, CVS Equine, made headlines by mandating that all equine vets, nurses, and techs wear a hard hat whenever handling or treating horses.
This policy, enacted across 21 equine practices, came after a three-year study with the University of Liverpool that laid bare the injury risks (90% of their clinicians had been injured; 25% of injuries sent someone to the hospital).
Now, whether on a farm call or in the clinic, CVS staff must clip on an equestrian-grade helmet if a horse, pony, or donkey is nearby. It’s a significant cultural shift, akin to when construction workers first started routinely wearing hard hats.
Initially, some of the older, wiser veterinarians resisted the idea, seeing helmets as cumbersome or a sign of inexperience. But the policy is evidence-based: many veterinarian head injuries happen from horse kicks or being knocked down, and hitting one’s head on the ground is a common cause of serious trauma.
A well built helmet can literally be the difference between a concussion or a skull fracture versus walking away with just a bruise. By embracing helmets, the UK group hopes to protect their staff and set a new standard industry-wide.
As one CVS director noted, veterinary medicine can borrow safety practices from other fields. If hard hats are standard on a construction site (with a lower injury rate), why not in a barn? This UK initiative appears to be a first-of-its-kind in terms of a large veterinary employer requiring helmets across the board. - Global ripple effect: The move from within the United Kingdom has sparked discussion in other countries. While no nationwide regulations compel vets to wear helmets yet, awareness is growing globally.
Some veterinary colleges have already been ahead of the curve. Veterinarians students at the University of Edinburgh’s Royal (Dick) School in Scotland are required to wear “jockey skull” helmets during equine handling classes.
The University of Nottingham likewise introduced helmets for students working with horses on the ground. These teaching institutions aim to ingrain safety habits in new vets from the start.
In the private sector, certain equine hospitals and studs have had their own rules: for instance, some breeding farms in the United States. mandate helmets and protective vests for anyone (vets, techs, handlers) during live breeding sessions, where the risk from fractious stallions is high.
Such policies have often been optional or site-specific, but the CVS mandate is encouraging others to consider formal PPE requirements. Conversations are popping up on veterinary forums and social media groups about whether “helmets for veterinarians” should become standard worldwide, especially for equine practitioners.
There is even work underway on designing better helmets tailored for equine veterinarians, who need something comfortable enough for all-day wear and that won’t spook horses. - Beyond helmets – safer practices: Equipment is only one piece; a cultural change in training and client cooperation is also key to safety. Professional bodies like BEVA have launched campaigns like “Don’t Break Your Vet,” which educate horse owners on how to help make vet visits safer (e.g. proper restraint, having a competent handler, keeping the environment controlled).
Veterinarians are learning to advocate for their own safety too – for instance, not hesitating to ask for a horse to be sedated or twitched, or to reschedule a procedure if conditions are too unsafe (such as a loose horse in a field with high wind).
There’s also a push for veterinarians to perform dynamic risk assessments: essentially a mental checklist before and during an exam (“Is the horse getting agitated? Are my exits clear? Do I have the right assistance and tools to do this safely?”).
While the job can never be risk-free, empowering equine veterinarans to set boundaries like refusing to proceed unless appropriate safety measures are in place , is a significant shift from the old mindset of always forging ahead.
The hope is that safety becomes as integral to equine practice as stethoscopes and hoof testers.
It’s worth noting that not everyone is instantly on board with these changes. Some seasoned equine clinicians and practitioners have been skeptical about helmets, arguing they’ve “managed fine for 20 years” without one.
Others worry that helmets could reduce their field of vision or scare nervous horses. However, attitudes are gradually shifting as the next generation comes in with safety expectations, and as evidence mounts that simple precautions can prevent devastating injuries.
The helmet debate in veterinary medicine has even been compared to seatbelt adoption in cars – once considered optional, now an obvious necessity.
Toward a Safer Future in Equine Practice
Equine veterinary work will never be free of risk as horses will always be powerful animals with a mind of their own. But clearly the risks don’t have to be “normal” to the degree they have been. The recent focus on injury data and prevention is a positive step.
By recognizing the scope of the problem – thousands of injuries, dozens of concussions, and too many close calls – veterinarians and their employers can take proactive steps to protect themselves without compromising care.
This means everything from wearing helmets and steel-toe boots to insisting on adequate restraint and assistance for difficult patients, to fostering a culture where vets feel supported in saying “no” to unnecessarily dangerous situations.
Most importantly, the conversation is open now. As I publish this article, I encourage our veterinary colleagues around the world to share their own experiences and safety tips in the comments on our facebook groups.
Our own Dr Sue Dyson is leading the field here, during a recent Lameness Workshop in Ocala, Florida, Dr Dyson shared her experience with near misses, injuries and how her protocol now is to always wear a helmet when performing lower limb nerve blocks.
Have you implemented new safety gear or protocols in your practice? Do you have a story of an injury that others could learn from, or a near-miss that changed how you work?
By talking openly about these incidents – rather than shrugging them off – we can all learn what not to do and how to do our jobs more safely. The goal is that fewer of us end up with broken bones, or black eyes, or worse, as simply “part of the job.”
Change won’t happen overnight, but it’s underway. From the UK’s helmet requirement to grass-roots campaigns and frank discussions among veterinarians, the profession is slowly shedding the notion that getting hurt by our patients is just business as usual.
No horse, no matter how valuable, is worth your life or livelihood. As i get older and my reactions become slower, I’ll be taking this safety precaution more seriously.
By normalising safety rather than risk, we ensure that we can continue doing the work we love – healing horses – and go home in one piece at the end of the day.
Sources:
- Vet Times –“Group introduces mandatory PPE for equine vets after study” (23 May 2025)
- VetSurgeon.org – “CVS makes PPE compulsory for equine vets” (22 May 2025)
- Tulloch et al. (2025), Preventive Vet. Medicine – “Understanding the safety culture in equine, production animal and mixed practices”
- CVS Group Press Release – “Largest ever study on veterinary workplace injuries…” (19 Nov 2024)
- Parkin et al. (2018), Equine Vet Education – “Occupational risks of working with horses: survey of equine vets”
- Equus Magazine –“Should veterinarians wear helmets?” (Fran Jurga, 2017)
- Occupational Medicine (UK) – “Pain, inconvenience and blame: defining work-related injuries in the veterinary workplace” (T. Furtado et al., 2024)
- DVM360 – “Animal Attacks Rank as Significant Workplace Risk” (D. Verdon, 2001)
- EquiManagement – “Injury Risk and Prevalence in Equine Practice” (A. Grice, Oct 2025)
- BEVA – “Injury: what can we do to protect ourselves?” (Alice Sheldon, 2013/updated)
- Horse Trust (UK) – Interview with Dr. Gemma Pearson (2025)







